Bladder Incontinence: Simple, Practical Help You Can Use Today
Bladder incontinence means you leak urine when you don’t want to. It happens to people of all ages. The good news: many cases improve with simple steps or basic treatments. This page explains why it happens, what to try yourself, and when you should see a doctor.
What causes bladder incontinence?
There are a few common types:
Stress incontinence — leaks when you cough, laugh, lift, or exercise. It often comes from weak pelvic floor muscles or after childbirth.
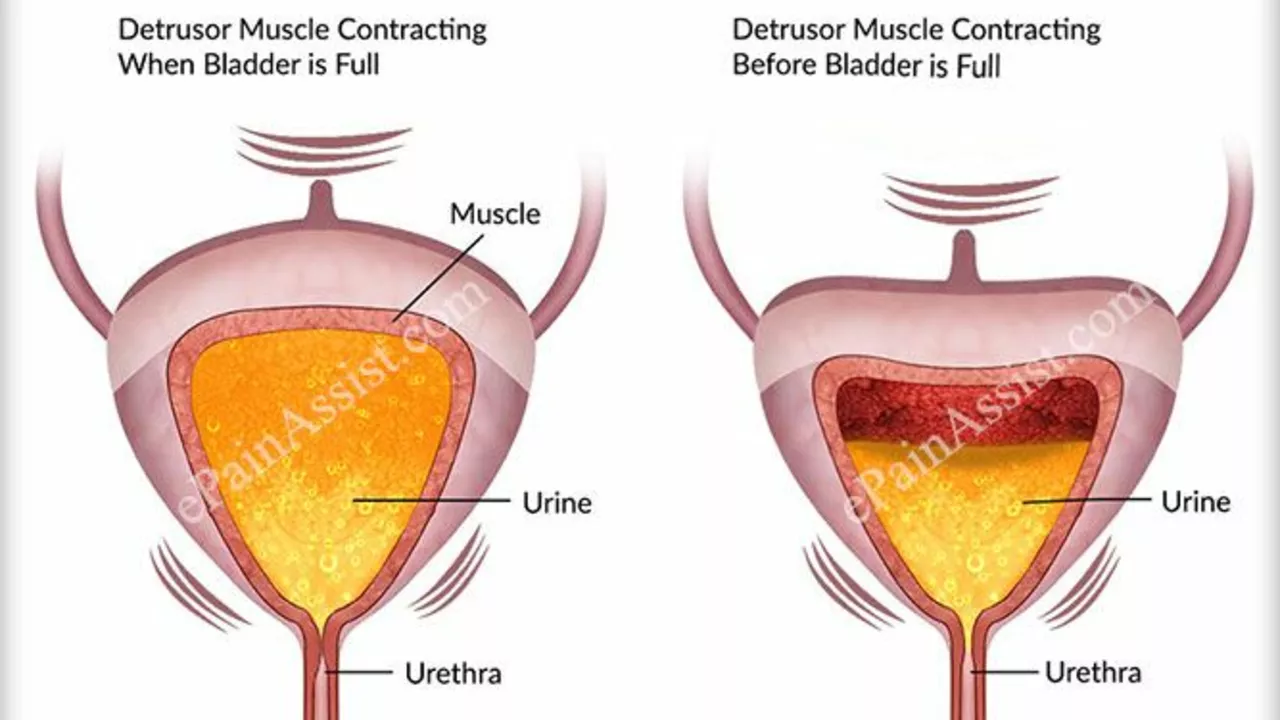
Urge incontinence — a sudden, strong need to pee and you can’t hold it. This ties to an overactive bladder or nerve signals that go wrong.
Overflow incontinence — the bladder doesn’t empty fully and dribbles. It can happen with prostate issues, certain medicines, or weak bladder muscles.
Other causes: urinary infections, constipation, some medicines (diuretics, sedatives), neurological issues (Parkinson’s, MS), obesity, and pelvic organ prolapse in women.
What you can do now
Start with easy, low-risk steps that help many people:
Keep a bladder diary. Track drinks, bathroom visits, and leaks for 3 days. This helps spot patterns and makes appointments more useful.
Pelvic floor exercises (Kegels). Tighten the muscles you’d use to stop peeing, hold 3–5 seconds, relax, repeat 10 times, three times a day. If you’re not sure you’re doing them right, a physiotherapist can help.
Bladder training. Try to increase the time between pees by a few minutes each day. This can lower urgency and frequency for urge incontinence.
Cut triggers. Reduce caffeine, alcohol, and fizzy drinks. Manage constipation and watch your fluid timing — don’t drink large amounts right before going out or bed.
Use pads or waterproof underwear for confidence while you work on longer-term fixes.
If these approaches don’t help, there are medical options. Doctors may offer medication for an overactive bladder, injections (botulinum toxin), pessaries for prolapse, or procedures like sling surgery for stress leaks. Tests your doctor might use include urine tests, post-void scan, and urodynamics to check bladder function.
You should see a doctor quickly if you have blood in urine, fever, sudden new severe symptoms, or if leaks start after a fall or surgery. Also see help if incontinence limits daily life despite self-care.
Talk to your GP about a plan that fits your routine. A pelvic floor physiotherapist and continence nurse are great allies. With the right steps, many people cut leaks dramatically and get their life back.
The impact of bladder and urinary incontinence symptoms on exercise and physical activity
In my recent research on bladder and urinary incontinence symptoms, I've discovered that these issues can have a significant impact on a person's ability to engage in exercise and physical activity. Many people experiencing incontinence tend to avoid activities that put pressure on their bladder, such as running, jumping, or even lifting weights. This can lead to a decrease in overall physical fitness and contribute to a sedentary lifestyle. It's important to address these symptoms with a healthcare professional and explore treatment options, as staying active is vital for our overall health and well-being. Don't let incontinence hold you back from maintaining a healthy lifestyle!
Read More