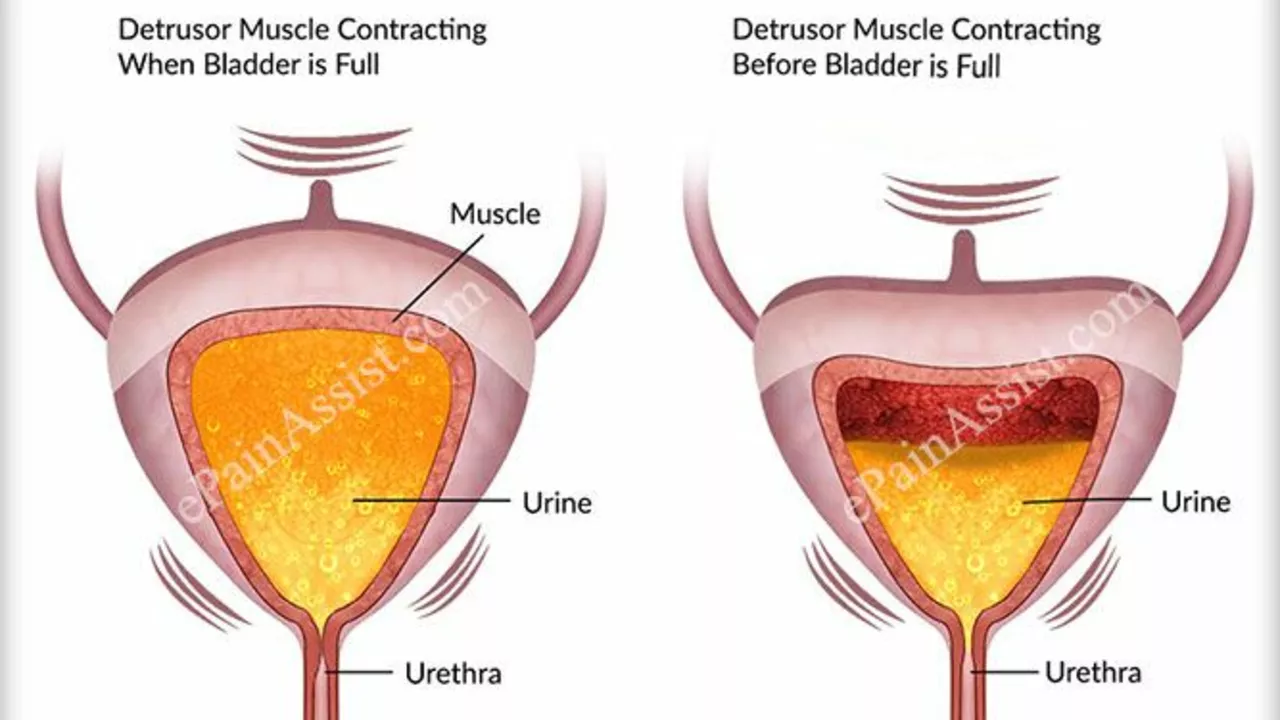
Urinary incontinence
Urinary incontinence is when you leak urine or can’t hold your bladder when you want. It’s common and treatable. Tired of leaking when you cough, laugh, lift, or run to the bathroom? Small changes and simple exercises often cut leaks.
Quick at-home steps
Start with easy, practical steps you can do today. Keep a bladder diary for three days: note what you drink, when you pee, how much, and any leaks. That helps your clinician and makes patterns obvious. Try pelvic floor exercises (Kegels): squeeze the muscles you would use to stop peeing, hold three to five seconds, then relax five seconds. Aim for ten reps, three times a day. If you can’t feel the muscles, try stopping midstream once to find them, but don’t make this a habit.
Bladder training can stretch how long you hold urine. Pick a schedule (for example every hour) and delay trips by fifteen minutes each week until you reach two to three hours. Cut back on bladder irritants like caffeine, alcohol, and artificial sweeteners. Spread fluids across the day and limit drinking two hours before bed to reduce nighttime trips.
Weight loss often reduces stress leaks in people with extra abdominal pressure. Quit smoking if you cough a lot — chronic coughing makes stress incontinence worse. Simple aids like absorbent pads or washable underwear let you stay active while you sort things out.
Medical options and tests
When home methods aren’t enough, medical options can help. Overactive bladder drugs such as anticholinergics or beta-3 agonists calm urgency but can cause dry mouth or constipation. Postmenopausal women may benefit from low-dose vaginal estrogen to improve tissue health. For stress incontinence, midurethral sling surgery is common and effective for many people.
Less invasive procedures exist too: botulinum toxin injections into the bladder reduce involuntary contractions for months, and sacral neuromodulation uses a small device to change bladder nerve signals. Men with prostate enlargement might need medication or procedures that lower obstruction and improve control.
Seek medical help right away if you have sudden incontinence, blood in urine, fever, severe pain, or new weakness or numbness. Those can be signs of infection, stones, or neurologic problems. Bring your bladder diary to appointments and be ready to describe timing, triggers, and how leaks affect your life.
Most people improve with the right mix of lifestyle, pelvic floor work, and medical care. Don’t accept leaking as normal—help is available, and small steps often lead to big improvements.
If home care fails after eight to twelve weeks, ask your doctor about tests. A urine test rules out infection or blood. Your clinician may measure leftover urine after peeing with an ultrasound and suggest urodynamic studies if the cause is unclear. A physiotherapist who specializes in pelvic floor can give biofeedback and hands-on training that speeds progress. For many people, combining therapy, lifestyle changes, and targeted treatments ends the problem.
Start with small goals: try Kegels twice daily, cut coffee, track progress in a diary and check regularly if leaks persist.
Urine Leakage and Sexual Health: What You Need to Know
Learn how urine leakage impacts sexual health, its causes, treatment options, and practical tips for maintaining intimacy and confidence.
Read MoreThe impact of bladder and urinary incontinence symptoms on exercise and physical activity
In my recent research on bladder and urinary incontinence symptoms, I've discovered that these issues can have a significant impact on a person's ability to engage in exercise and physical activity. Many people experiencing incontinence tend to avoid activities that put pressure on their bladder, such as running, jumping, or even lifting weights. This can lead to a decrease in overall physical fitness and contribute to a sedentary lifestyle. It's important to address these symptoms with a healthcare professional and explore treatment options, as staying active is vital for our overall health and well-being. Don't let incontinence hold you back from maintaining a healthy lifestyle!
Read More