Medical Research: Clear, Practical Summaries on Drug Safety
Chemotherapy and other strong drugs save lives, but they can also affect organs like the liver. Want straight answers from the latest research without the technical overload? This category breaks down studies into useful takeaways you can use in the clinic or discuss with your care team.
What you’ll find here
Short, focused summaries of recent studies, case reports, and reviews. We highlight real risks, who’s most likely to be affected, and practical steps to reduce harm. Each post points to the original research so you can check methods and numbers if you want the full details.
Think of these pages as a quick bridge between dense papers and everyday decisions. We translate study designs, sample sizes, and outcomes into clear actions: which tests to order, monitoring schedules, and simple changes that lower risk.
Featured: Melphalan and the liver — what the research says
One recent post looks at Melphalan, a chemotherapy drug used in certain cancers. Studies and clinical reports show Melphalan can cause hepatic injury in some patients. The risk looks higher with high-dose regimens, combination therapies, or when patients already have liver disease. The research points to measurable liver test changes—ALT, AST, bilirubin—and, in rare cases, clinically significant liver dysfunction.
What helps? The studies recommend clear steps: check baseline liver function tests before starting Melphalan, repeat labs during treatment, and lower doses or pause therapy if liver enzymes rise sharply. That’s simple: baseline liver panel, weekly checks during intensive cycles, and at least one follow-up after finishing treatment. If someone takes other liver-risk drugs (like high-dose acetaminophen or known hepatotoxic chemo), consider alternatives or tighter monitoring.
Some trials and case series explored protective measures. Agents such as ursodeoxycholic acid or N-acetylcysteine have been tested in related liver injury settings and appear promising in small studies, but evidence is limited. The practical takeaway: discuss potential protective strategies with your oncology team rather than starting supplements on your own.
If you’re a clinician, use the detailed post to guide consent conversations and monitoring plans. If you’re a patient, ask your provider about liver tests before and during treatment, about symptoms to report (jaundice, severe fatigue, abdominal pain), and about medication interactions.
Want more posts like the Melphalan piece? Browse this category for drug safety reviews, short trial summaries, and clear management tips. We link each summary to the original studies so you can dig deeper when you need the full evidence.
Questions or a paper you want summarized? Send it our way. We aim to make medical research usable—no fluff, just practical steps you can act on now.
FDA Safety Alerts: 2025-2026 Warnings, Guidance Changes, and Consumer Actions
An overview of the 2025-2026 FDA safety alert changes, covering medical device expansions, drug warnings, and how consumers can stay protected.
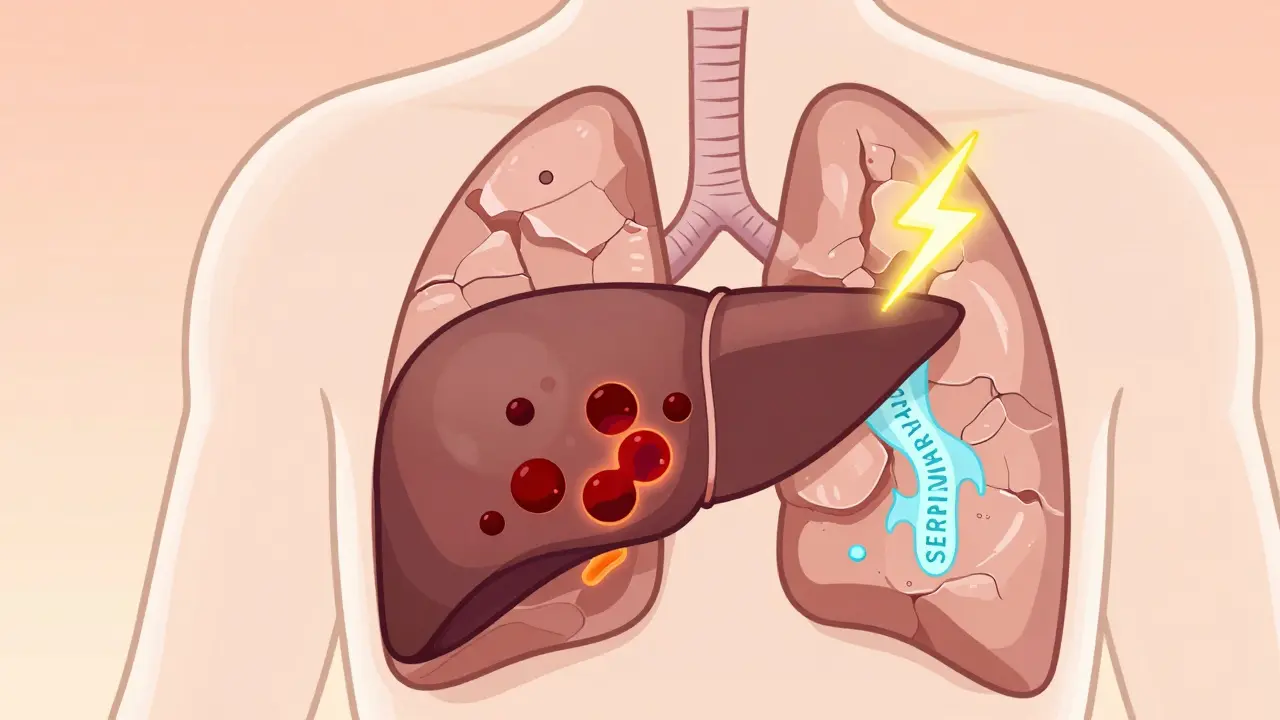
Read MoreAlpha-1 Antitrypsin Deficiency: The Genetic Cause of Early-Onset COPD and What You Can Do
Alpha-1 Antitrypsin Deficiency is a genetic cause of early-onset COPD that affects 1 in 2,000 people. Often misdiagnosed, it requires specific testing and lifelong treatment. Learn how to spot it and what treatments are available.
Read MoreAutoimmune Uveitis: How Steroid-Sparing Therapy Protects Your Vision
Autoimmune uveitis can cause permanent vision loss if untreated. Steroid-sparing therapies like Humira, methotrexate, and cyclosporine help control inflammation without the dangerous side effects of long-term steroids.
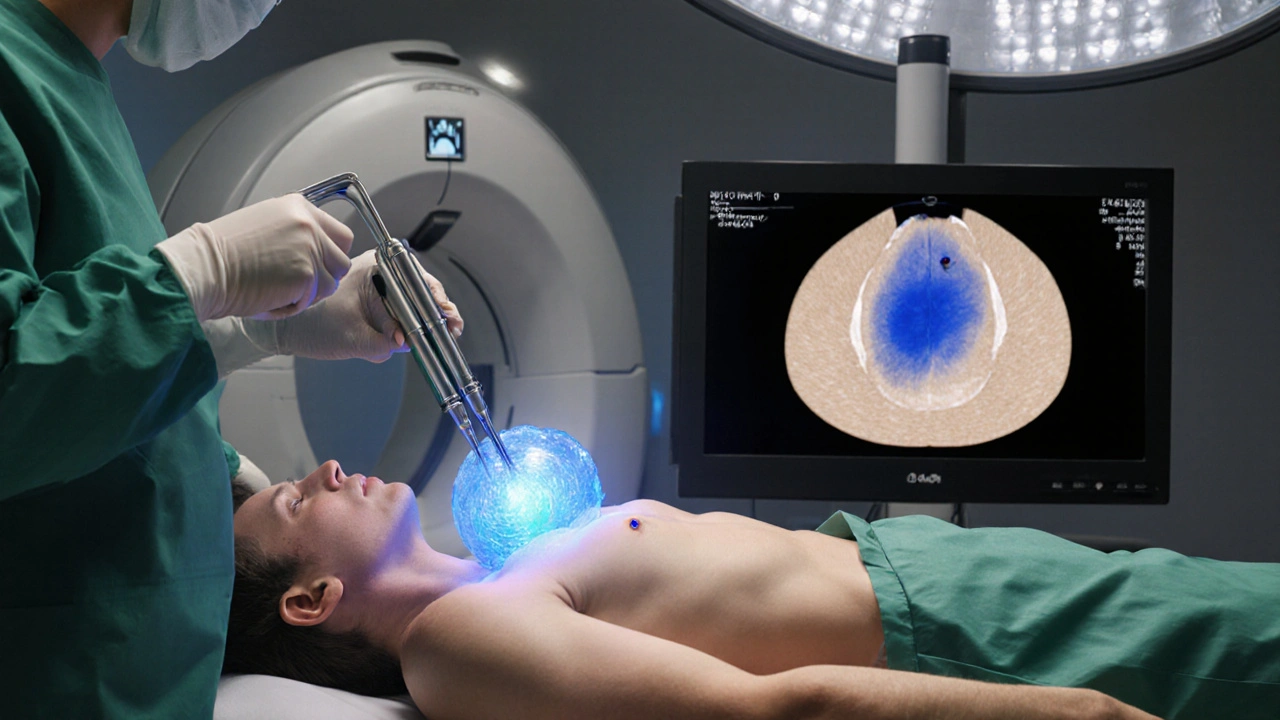
Read MoreCryoablation for Advanced Renal Cell Carcinoma: Benefits, Risks & Outcomes
Explore how cryoablation works for advanced renal cell carcinoma, review clinical evidence, compare it to other ablation methods, and learn patient selection, risks, and future trial updates.
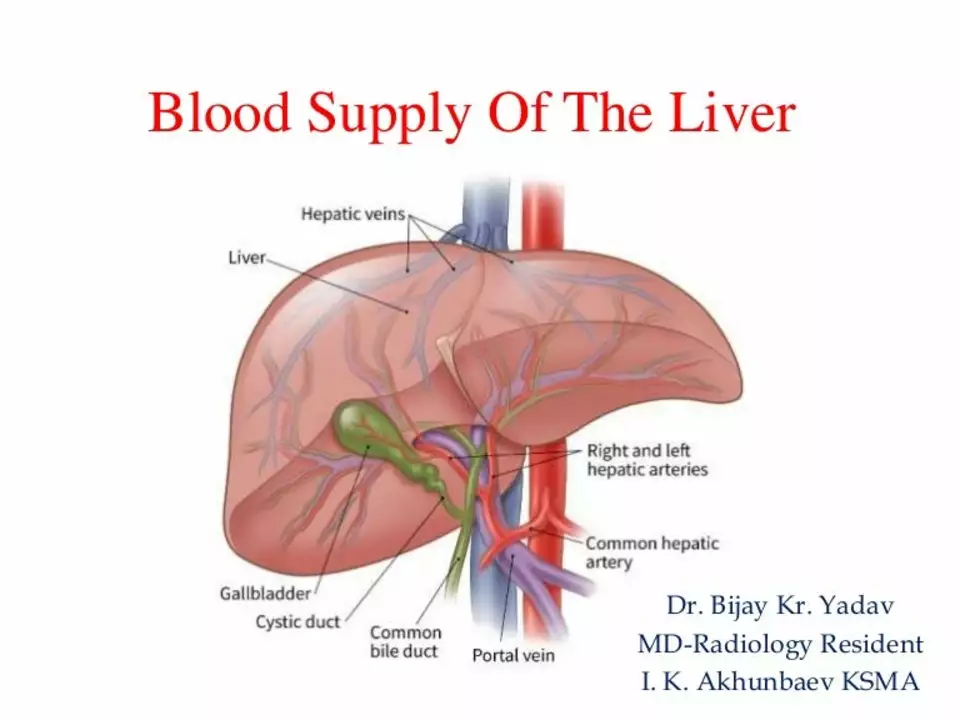
Read MoreMelphalan and the Liver: Understanding Hepatic Toxicity and Management Strategies
In my recent research, I delved into the effects of Melphalan on the liver, specifically focusing on hepatic toxicity and management strategies. I found that Melphalan, a chemotherapy drug, can cause liver damage in some patients, which is a concerning side effect. However, there are ways to manage and minimize these risks, including monitoring liver function tests and adjusting dosages. Additionally, some studies suggest that using other medications alongside Melphalan may help protect the liver. Overall, it's essential for healthcare providers and patients to be aware of these risks and management strategies to ensure the safe use of Melphalan.
Read More