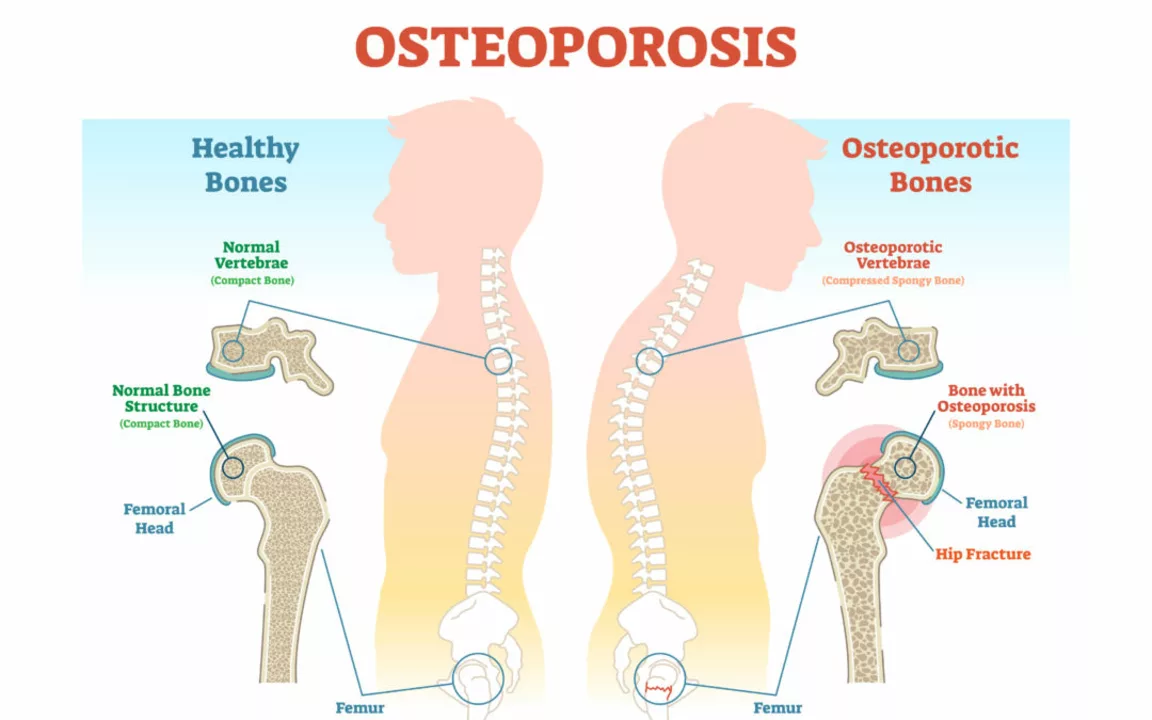
Bone Health: Practical Steps to Keep Your Bones Strong
One in three women over 50 will break a bone due to osteoporosis. That’s a startling number, but you can cut your risk with clear, everyday steps. This guide gives straightforward tips on diet, exercise, tests, medication, and common drug interactions so you know what to do next.
Diet first: aim for total calcium of 1,000–1,200 mg daily depending on age (1,200 mg for women over 50 and men over 70). Get calcium from dairy, fortified plant milks, canned salmon with bones, tofu, and leafy greens. Vitamin D helps your body absorb calcium — aim for about 800–2,000 IU a day, more if your doctor finds a deficiency. Consider vitamin K2 (MK‑7, 90–200 mcg) for bone metabolism, but check with your clinician if you take warfarin or other blood thinners.
Move smart: exercise that builds bone
Weight‑bearing activities (walking, stair climbing, dancing) and resistance training (bands, weights) help maintain bone density. Try 30 minutes most days and strength sessions 2–3 times per week. Balance and mobility work — like tai chi or single‑leg stands — reduce fall risk. If you’re new to exercise, start light and build up; ask a physiotherapist for a simple plan tailored to injuries or arthritis.
Know when to test and treat
Ask for a DEXA bone density scan if you’re a woman 65+, man 70+, or younger with risk factors (long steroid use, low body weight, early menopause, or family history). If bone density is low, common treatments include bisphosphonates (alendronate, risedronate), denosumab (Prolia), and SERMs like raloxifene. Each has benefits and side effects — bisphosphonates can irritate the esophagus and rarely cause jaw problems; denosumab needs a clear plan before stopping. Talk to your doctor about the right option for you.
Medication interactions and risks matter. Long‑term steroid use causes bone loss — discuss preventive treatment early. Proton pump inhibitors have been linked to higher fracture risk when used long term. Calcium supplements can interfere with absorption of some antibiotics and thyroid meds, so space doses by two hours. Always tell your pharmacist and doctor what supplements and prescriptions you take.
Practical daily tips: make your home fall‑safe (good lighting, remove loose rugs, install rails), keep protein intake adequate (about 1.0–1.2 g/kg for older adults), and limit heavy alcohol and smoking. If you have dental surgery planned, tell your dentist if you take osteoporosis drugs.
Want a quick next step? Book a DEXA if you meet screening criteria, review your medications with a pharmacist, and add two strength sessions to your week. Small, consistent changes protect your bones much more than quick fixes.
When choosing supplements, pick reputable brands with third‑party testing (USP, NSF) and follow label doses. Avoid megadoses of calcium or vitamin D unless prescribed after checking blood levels. Recheck bone density every 1–2 years if you’re on treatment. If you’ve had a fracture, ask for a fracture liaison service referral — many hospitals have a program to prevent the next break.
Start today.
Osteodystrophy and Fracture Risk: What You Need to Know
As someone who's been researching osteodystrophy and fracture risk, I've learned a lot about this important topic. Osteodystrophy is a bone disorder that can lead to weakened bones and an increased risk of fractures. It's essential to be aware of the risk factors and symptoms so we can take preventive measures to protect our bone health. In my research, I've discovered that maintaining a balanced diet, participating in regular exercise, and seeking medical advice when necessary can make a significant difference in managing this condition. Stay informed and proactive to give your bones the best chance at staying strong and healthy!
Read More